Category: Nurse’s Corner

Medical Team Supports Mesothelioma Patients in Making Care Decisions
According to a recent survey, 64% of respondents believe they could be making more decisions about their health and wellness. This national survey emphasizes the importance of empowering individuals with information within a dynamic healthcare environment. The survey by the National Council of Patient Information shows how important communication and trust is with your medical team. But unfortunately, more and more patients diagnosed with mesothelioma turn to the internet. This one-sided approach to learning about the disease can lead to unrealistic expectations, for both the patient and family.
This past week a man who had surgery a year ago, a pleurectomy, for malignant pleural mesothelioma was re-admitted to the hospital. His course has been complicated over the last year, and emotionally it has been a challenge. He has undergone chemotherapy, and fell and sustained bruises while being on a blood thinner. After surgery, both he and his wife felt that progress was way too slow. He was disappointed in how he felt. He wanted more out of himself physically and looked upon his slow progress as a failure on his part.
He was readmitted and found to have metastatic disease – his mesothelioma had spread. He was offered the options best suited him by his team. He could restart chemotherapy or he could elect to go home with hospice. Armed with his options, he was going home to think about his choices. Did he want to go through another round of chemotherapy or did he want to choose hospice? This is a very personal decision that he and his family had to make.
In order to make healthcare decisions, all questions must be answered, the information must be understood, and all communication must be clear. Whatever decision the patient makes will be fully supported by the medical team. As his journey continues with mesothelioma, the choices he makes will impact he and his family. What are his values? What does he value in his life? His decisions made with his family, and his medical team, will be based on what he wants.
Know more about Mesothelioma and how you can deal with it.
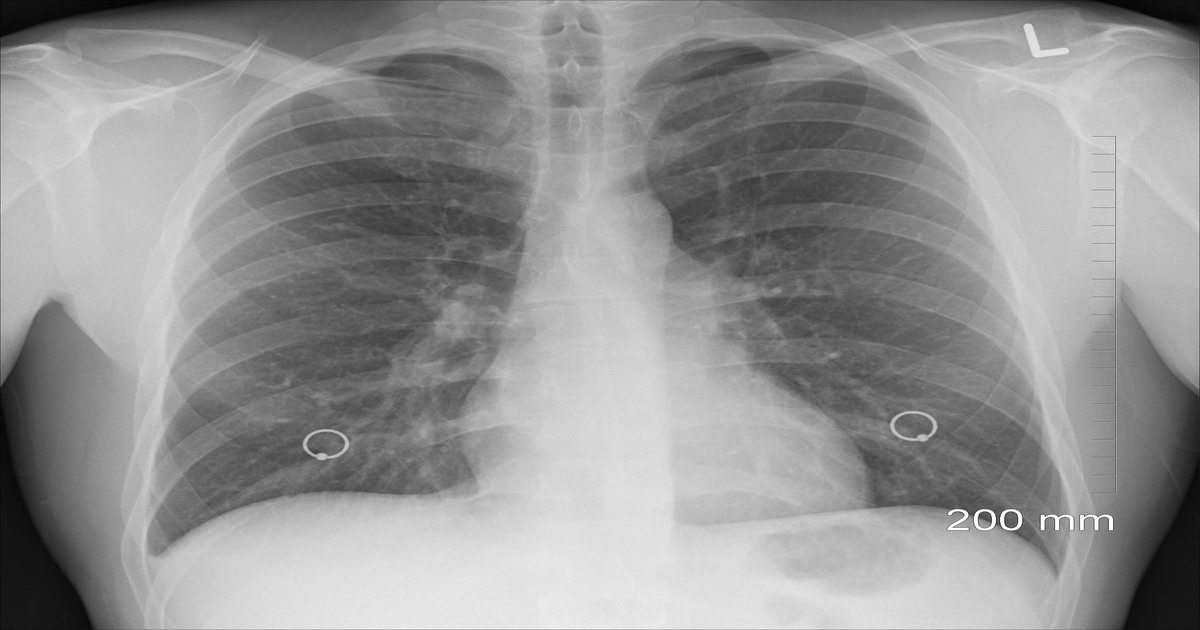
Mesothelioma Nurse Explains Pleural Effusion
Obtaining a diagnosis of malignant pleural mesothelioma is difficult. The diagnosis is often made after many other more common diseases are ruled out. One of the presenting symptoms can be pleural effusion, or excess fluid in the chest cavity. It is a common symptom with one study placing it as high as 90 % in a group of patients diagnosed with malignant pleural mesothelioma.
What is pleural effusion? The pleura is a thin layer that surrounds the lungs. The outer layer is the parietal pleura, and the inner layer is the visceral pleura. Lubricating the layers in the space in between is a small amount of fluid called the pleural fluid. The pleural fluid functions to lubricate the two layers so they can slide against each other when we breathe. In healthy people, the pleural fluid is usually about a teaspoon. With a pleural effusion, the fluid builds up and separates the lung from the chest wall, making it difficult to breathe. Some of the more common conditions that a person could have to cause pleural effusion are pneumonia, heart failure, low level of protein in the blood, cirrhosis of the liver, rheumatoid arthritis, systemic lupus erythematosus (SLE), and mesothelioma.
Shortness of breath is most often the reason many patients diagnosed with malignant pleural mesothelioma seek medical attention. For many patients, initially, they undergo a procedure to drain the fluid called a thoracentesis. Many patients who are eventually diagnosed with mesothelioma have this procedure done more than once. Once the diagnosis is made and treatments begin, the effusions can be less of an issue as the symptom is managed with the disease.
When pleural effusions continue to be an issue due to the advancement of disease, or whatever the reason may be, there are options for managing the patient‘s discomfort. One of these options can be a catheter placement in the chest that allows the patient to drain the fluid at home and not come to the hospital for the thoracentesis procedure. Insertion of these catheters can often give the patient and family more time to spend at home as opposed to going to the hospital. If you or your loved one is in the situation that requires frequent thoracentesis procedures, this could be an option.
This past week a patient brought up placement of a pleural catheter as he was considering it. He had weighed the pros and cons and decided to delay placement because it was summertime and he enjoyed going into the water. As mesothelioma becomes a chronic disease it is gratifying to see options that patients have depending on their needs and their quality of life goals.
Photo Credit: Dr. James Heilman via Wikipedia

The Results of Mesothelioma Research are Worth The Wait
At a recent conference, a distinguished mesothelioma specialist was explaining how mesothelioma is a very complicated, aggressive cancer and that every case is different. He continued, by saying that while progress is ongoing it can already be seen in certain segments of patients with mesothelioma. Intellectually I know he is right, but all my patients have names and stories, and emotionally I pray that they will be the ones that benefit from the progress. Today, I saw firsthand the results of some of that progress.
Three years ago Mr. Z had an extrapleural pneumonectomy for his mesothelioma. His recuperation was complicated. He had a supportive brother and sister. He had not married and relied on his siblings and nieces and nephews for emotional support. Throughout his stay in the hospital and in the numerous rehabs they were with him.
We had visited him in multiple rehabs, talked with his sister multiple times, encouraged him to continue to fight. The last time I saw him was around two years ago, he was being released from the rehab and was headed home. He lived downstairs in a two-family house where his sister and her family lived upstairs.
Today at work, I was assisting another nurse and thought the patient on the stretcher looked vaguely familiar. When he said his name, and I asked him where he was from, it registered. I thought he was his brother: he looked wonderful! He had gained weight, was home and had been home for a couple of years. He was living with some of the challenges that mesothelioma and a long recovery had left him, but he was at home doing what he wanted. He was enrolling in a clinical trial and was going to have a procedure to see if he was a candidate. As expected his sister and brother were with him.
After the procedure, I saw his sister and brother. After a big hug and a few tears, his sister said she remembered our conversations and my encouragement, and she shared how well her brother had been doing. Her reflection after three years that although it had taken a long while to get to this point, they were glad to have stayed the course. Now, they were attempting to enroll him in a clinical trial that was a result of the progress that we had been following over the years.
As they were leaving they were discussing when to order Thai food and the best time of day to avoid the rush. Sometimes progress is slow and research takes time- but it is so worth it!
Photo Credit: National Cancer Institute
Memorial Services Honor Mesothelioma Victims
Once a year the International Mesothelioma Program at Brigham and Women’s Hospital in Boston holds a memorial service for patients who lost their battle to the disease. It is not easy for families to come back to a place that had such an emotional connection for them and their loved ones, who lost their battle with mesothelioma.
For caregivers and families alike it is a very emotional day. For the staff, it is one of the most important programs we can attend each year. It reminds all of us what has been lost to this disease. It allows us to put a face and names to those who have fought mesothelioma, to become invigorated to work harder in memory of these who have died, and to reconnect with families who have a lost a piece of their heart to a cruel cancer.
[expert_info author=”Tagore”]“Say not in grief that she is no more but say in thankfulness that she was. A death is not the extinguishing of a light, but the putting out of the lamp because the dawn has come.” [/expert_info]Memorial Day is another day set aside for remembering and honoring those who have died. We reflect and pay our respect and gratitude to those who have sacrificed their lives for our country. Whether it be in battle defending our country, or an insidious disease that those who lived are diagnosed with years later. Whether it is their loss of life from the effects of agent orange or asbestos exposure, those who sacrificed for our country deserve our unending gratitude.
Approximately 30% of mesothelioma patients who are diagnosed are U.S. veterans. With the time of exposure to asbestos to the time of developing mesothelioma taking from 15-60 years, this disease is a killer of our service men and women.
Memorial Day and the annual Memorial Service at Brigham and Women’s are held this time of year every year, and every year we pause and vow never to forget those who have died.
Who is the Patient?
With such a devastating disease as mesothelioma you would think it would be easy to pick out who is the patient. Not necessarily. At a recent mesothelioma conference I attended there was an empty seat at a table with two couples who were already seated. I joined them, and as our conversation progressed it became apparent that both couples had one partner who had mesothelioma and the other who was the very supportive spouse. I had to ask both couples who was the patient.
The first couple were in there 70’s, friendly, and both appeared very fit. The man was the patient. He had recently undergone a pleurectomy and suffered some complications, but he was now doing well. His life is full of activities and he said he tires more easily than before surgery. His wife spoke of how she encourages him to rest every day, but some days he won’t give in. The man said he is cautious about how much weight he will lift. He tries not to lift anything larger than 10 pounds.
The second couple at the table were in their early 60’s. The woman was the mesothelioma patient. She had been diagnosed over two years ago, had never had surgery, and she had been treated with chemotherapy. She reported that she had never experienced shortness of breath, and overall she felt very well. Her biggest complaint was fatigue. It was not constant but on occasion she felt wiped out. Her appetite was good, and she looked wonderful. In a strange way she was grateful for the diagnosis. Mesothelioma had given her and her husband time to do what they wanted now- not in the future. They had done some traveling, visited their children, and made it a point to enjoy life to the fullest now.
Mesothelioma is a rare disease. It is also a disease that affects everybody differently. Every mesothelioma tumor is different, as is every patient and family that it affects. Knowing these facts, and seeing it play out with two couples at a mesothelioma conference, was very inspiring to me.
Watching these two couples, who did not know each other before the conference, sharing stories and supporting each other, is what being part of a sharing, supportive community is all about.
Free Mesothelioma Patient & Treatment Guide
We’d like to offer you our in-depth guide, “A Patient’s Guide to Mesothelioma,” absolutely free of charge.
It contains a wealth of information and resources to help you better understand the condition, choose (and afford) appropriate treatment, and exercise your legal right to compensation.
Download Now